Sepsis is a medical emergency requiring immediate identification and treatment
Sepsis is one of the leading causes of death worldwide. It is a life-threatening condition caused by a dysregulated host response to infection, which can progress to multiple organ dysfunction, septic shock and even death 1.
Every hour counts in sepsis. It’s a medical emergency that requires immediate diagnosis because any delay in treatment can dramatically reduce the chances of survival 2.
Unfortunately, today’s standard of care means that sepsis is often diagnosed too late
Sepsis early warning signs and symptoms, such as fever, chills, nausea, fatigue, pain, etc., are generic and non-specific, making it extremely challenging to differentiate sepsis from other conditions.
However, research shows that the early detection of sepsis with timely, appropriate interventions increases the likelihood of survival.
Pancreatic Stone Protein (PSP) is an early marker of sepsis
PSP is a protein biomarker produced by the pancreas and secreted in response to sepsis-related organ dysfunction.
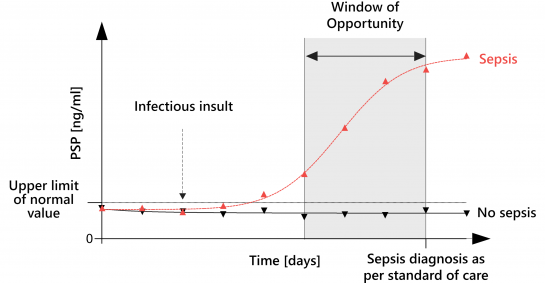
PSP has shown great accuracy as an early warning sign of sepsis, increasing up to 3 days before overt clinical signs and symptoms appear 3. Abionic brings together an ultra-rapid nanofluidic-based diagnostic platform and the PSP biomarker to offer a unique bedside test for the earliest and immediate detection of sepsis. Its availability at the point of care (POC) on the abioSCOPE® device will enable the timely initiation of optimal treatments, thanks to a more accurate identification of sepsis.
LISTEN TO THE EXPERTS :
Discover presentations from international speakers, highlighting the role of Pancreatic Stone Protein in Sepsis Management
Early diagnosis of sepsis - Dr François Ventura - 2023
The Use of Biomarkers for Sepsis and Antimicrobial Resistance Management - Dr Philippe Eggimann - 2022
Guiding Clinical Care Using PSP - Webinar - 2022
Identification of Sepsis Up to 72h in Advance - 2022
Real World Evidence for Implementing PSP measurements at the Point-of-Care - 2021
CURIOUS TO LEARN MORE?
Discover how multiple clinical studies have demonstrated the clinical benefits of PSP.
FAQs
The early warning signs and symptoms of sepsis are typically not specific enough to permit early identification, allowing it to rapidly progress towards septic shock when left undiagnosed. For every hour that goes by where the patient doesn’t receive suitable antibiotic therapy, the chance of survival decreases by 8% 2.
PSP increases rapidly in blood up to 72 hours before the clinical diagnosis of sepsis, operating as an alarm signal for physicians to act upon. In addition to the diagnostic value of the PSP biomarker for sepsis, its 24/7 availability to be used at the patient’s bedsides offers an additional opportunity to closely monitor patients at risk of sepsis.
The PSP test, used in conjunction with the entire clinical assessment of the patient, aids in the early recognition of nosocomial sepsis in adults. This early knowledge that a patient is likely to develop sepsis may prompt a closer and more tailored patient management and help prevent severe complications and even death.
PSP is recommended as an aid in the early diagnosis of sepsis in critically ill adult patients with suspected sepsis, or at risk of developing sepsis. Serial measurements on a daily basis can allow for the early detection of acute changes in the PSP blood concentration.
The test should be performed immediately after blood collection (recommended) but is stable for up to 4 hours after collection when kept at room temperature or refrigerated.
References